Researching Stage 3 Lyme Disease Neurological Symptoms:When Borrelia Reaches the Brain
Most people know Lyme disease as the illness you get from a tick bite.
They picture the bull’s eye rash, a round of antibiotics, and a clean bill of health.
What they do not know is that for a significant number of people, that is not where the story ends.
When Lyme disease goes undetected or inadequately treated in its early stages, the infection can disseminate throughout the body and eventually reach the central nervous system.
This is what clinicians call late disseminated Lyme disease, or stage 3.
And when Borrelia reaches the brain, the symptoms that follow can be some of the most debilitating and most misunderstood in all of medicine.
Brain fog so thick you cannot finish a sentence.
Memory gaps that leave you standing in a room with no idea why you are there.
Depression that does not respond to antidepressants.
Anxiety that feels physical as much as emotional.
Cognitive decline that doctors cannot explain.
Stage 3 Lyme disease neurological symptoms are real, they are documented in the clinical literature, and they are being missed every single day by practitioners who are not looking for them.
This post is about why that is happening and what you need to know.
The bull’s eye rash appears in fewer cases than most people think.
The absence of a rash does not mean the absence of infection.
And by the time the stage 3 Lyme disease, neurological symptoms appear, the infection may have been quietly progressing for months or years.
While tick bites are the established route of Lyme disease transmission, some researchers and Lyme-literate clinicians have raised questions about whether other vectors may play a role.
What is clear is that exposure is more widespread than many people realize and that standard testing frequently fails to catch the infection, regardless of how it was acquired.
Understanding the Three Stages of Lyme Disease
Lyme disease progresses through three recognized stages, each reflecting how far the infection has spread through the body.
Stage 1 is early localized infection, typically occurring within days to weeks of a tick bite.
This is when the classic erythema migrans rash may appear, along with flu-like symptoms including fever, chills, fatigue, muscle aches, and headache.
Stage 2 is early disseminated infection, occurring weeks to months after the initial bite.
At this stage the bacteria have begun spreading beyond the skin into the bloodstream and tissues.
Symptoms can include multiple rashes, facial palsy, heart rhythm problems, nerve pain, and the beginning of cognitive difficulties.
Stage 3 is late disseminated Lyme disease, which can occur months to years after the original infection.
By this stage, Borrelia has had the opportunity to reach the joints, the heart, and critically, the nervous system and the brain.
Stage 3 Lyme disease neurological symptoms are among the most complex and difficult to diagnose because they overlap with so many other conditions.
Depression, anxiety, cognitive impairment, memory loss, and neurological dysfunction can all be attributed to other causes, and frequently are, while the underlying infection goes unaddressed.
Why So Many People Reach Stage 3 Without a Diagnosis
There is a common assumption that if you have Lyme disease you will know about it.
The reality is more complicated.
The bull’s eye rash, while the most recognized symptom of early Lyme, does not appear in every case.
Estimates vary but a meaningful percentage of people with confirmed Lyme disease never develop the classic rash at all.
Without that visual marker, early Lyme is easily missed.
The flu-like symptoms of stage 1 are attributed to dozens of other illnesses.
The tick bite itself may go unnoticed, particularly with nymph-stage ticks which are roughly the size of a poppy seed. And in some cases there was no tick bite.
And then there is the testing problem, which we will get to in section two, because it is central to understanding why stage 3 Lyme disease neurological symptoms are so frequently misdiagnosed.
The Master of Stealth: How Borrelia Hides from Testing and Treatment
Borrelia burgdorferi is not a straightforward pathogen.
It is one of the most sophisticated bacterial organisms ever studied, and its ability to evade both the immune system and standard diagnostic testing is well documented in the peer-reviewed literature.
Understanding this is essential to understanding why stage 3 Lyme disease neurological symptoms so often go unrecognized and untreated.
Biofilm Formation
One of Borrelia’s most important survival strategies is its ability to hide inside biofilm.
Biofilm is a protective matrix, a kind of biological fortress made of extracellular polysaccharides, that the bacteria construct around themselves.
Inside the biofilm, Borrelia is sheltered from both immune attack and antibiotic penetration.
Research published in peer-reviewed journals has confirmed the presence of Borrelia biofilm in human skin tissue, and biofilm-like structures have been observed in key tissues, including joints, skin, and the central nervous system, in animal models of Lyme disease.
Critically, biofilm formation directly affects diagnostic testing.
Standard blood tests for Lyme disease detect antibodies produced by the immune system in response to the infection.
When Borrelia is sheltered within biofilm, it may alter antigen expression or suppress the immune response entirely, resulting in antibody levels that fall below detectable thresholds.
Basically, Borrelia hides in the biofilm, going unrecognized.
The key, then, is to use methods that coax it out of its hiding place so it can be found during a test.
Another thing to note is that spirochetes enjoy feeding on hyaluronic acid, so if you take this supplement, it can bring them out as well.
This is why Lyme affects the joints.
A patient with an active Lyme disease infection can receive a negative test result if the bacterium hides well.
Not because the infection is not there.
Because the bacteria have hidden themselves too well for the test to find.
Cistus tea is can help break up biofilms in the gut. You can read more about Cistus in our article here.
However, breaking up biofilm and how to do it safely is nuanced and warrants a whole other article, which I have covered to some degree in other Lyme articles.
Antigenic Variation
Beyond biofilm, Borrelia uses another remarkable evasion strategy called antigenic variation.
Through a process of continuous gene recombination, Borrelia constantly changes the surface proteins it presents to the immune system.
By the time the immune system has produced antibodies to recognize one surface protein, the bacteria has already changed its coat and become unrecognizable to those antibodies.
Basically, it is so stealthy it can cloak.
This is one reason why the immune response to Borrelia never fully clears the infection in many patients, and why the standard antibody-based testing can miss it entirely.
The bacteria the immune system learned to recognize is no longer the bacteria that is present.
The Testing Gap
The standard two-tier testing protocol recommended for Lyme disease uses an ELISA screening test followed by a Western Blot confirmatory test.
Both tests detect antibodies rather than the bacteria directly.
The sensitivity of standard Lyme testing has been documented to be highly variable, with some research showing sensitivity as low as 34 to 70 percent depending on the stage of infection and the laboratory performing the analysis.
This means a significant number of patients with genuine Lyme infections receive false negative results.
They are told they do not have Lyme disease.
They leave the doctor’s office without answers.
And the infection continues to progress.
Comprehensive testing through laboratories that use expanded panels, direct antigen detection methods, and co-infection screening offers a more complete picture.
But these tests are not always offered, not always covered by insurance, and not always known to the treating physician.
A negative Lyme test is not the same as a Lyme-free result. The stealth mechanisms of Borrelia make standard antibody testing an unreliable tool for ruling out infection, particularly in late stage disease.

When Borrelia Reaches the Brain: Stage 3 Lyme Disease Neurological Symptoms
Neuroborreliosis, the term used to describe Lyme disease affecting the nervous system, is a recognized clinical diagnosis with a documented spectrum of neurological and psychiatric manifestations.
When Borrelia crosses the blood-brain barrier and establishes itself in central nervous system tissue, the consequences can be profound and far-reaching.
How Borrelia Enters the Brain
Borrelia burgdorferi has been shown in research to invade a variety of human cell types including endothelial cells, which line the blood vessels, neural cells, and neuroglial cells.
Its ability to penetrate the blood-brain barrier and establish itself in neurological tissue has been confirmed in both animal studies and post-mortem human brain analysis.
Once inside the central nervous system, Borrelia triggers a neuroinflammatory response.
Research has documented that Borrelia infection is associated with elevated levels of proinflammatory cytokines, including Interleukin-6, Interleukin-8, Interleukin-12, and Interferon-gamma.
The bacteria’s surface proteins elicit anti-neuronal antibodies that can disseminate from the periphery into the brain, creating persistent inflammatory effects that alter brain chemistry, neurological signaling, and cognitive function.
The Brain Autopsy Evidence
Perhaps the most sobering evidence of Borrelia’s neurological impact comes from post-mortem brain analysis.
A 2023 study published in the International Journal of Molecular Sciences examined the brain tissue of a patient born in 1996 who had been diagnosed with Lyme disease as a child following an erythema migrans rash.
Despite receiving antibiotic treatment, his condition progressively worsened over the following thirteen years.
He developed the experience of Lyme disease brain fog, cognitive deficits, reduced psychomotor performance, and difficulties with concentration.
He was eventually hospitalized in a psychiatric clinic and prescribed multiple psychiatric medications.
None of it helped.
After his death, PCR testing of multiple regions of his brain confirmed the presence of not one but two species of Borrelia spirochetes, Borrelia burgdorferi sensu stricto and Borrelia garinii, detected in distinct areas of brain tissue.
The infection had survived years of antibiotic treatment, persisted in the brain, and driven a clinical picture that was managed as a primary psychiatric condition until the very end.
Columbia University researchers published similar findings, detecting Borrelia burgdorferi spirochetes in the brain and spinal cord of a woman who had experienced progressively worsening neurological symptoms and personality changes following a Lyme disease diagnosis, eventually dying of Lewy body dementia.
These findings matter because they confirm what many Lyme-literate clinicians have observed in practice: Borrelia can persist in the brain despite treatment, and its neurological consequences can be devastating when missed.

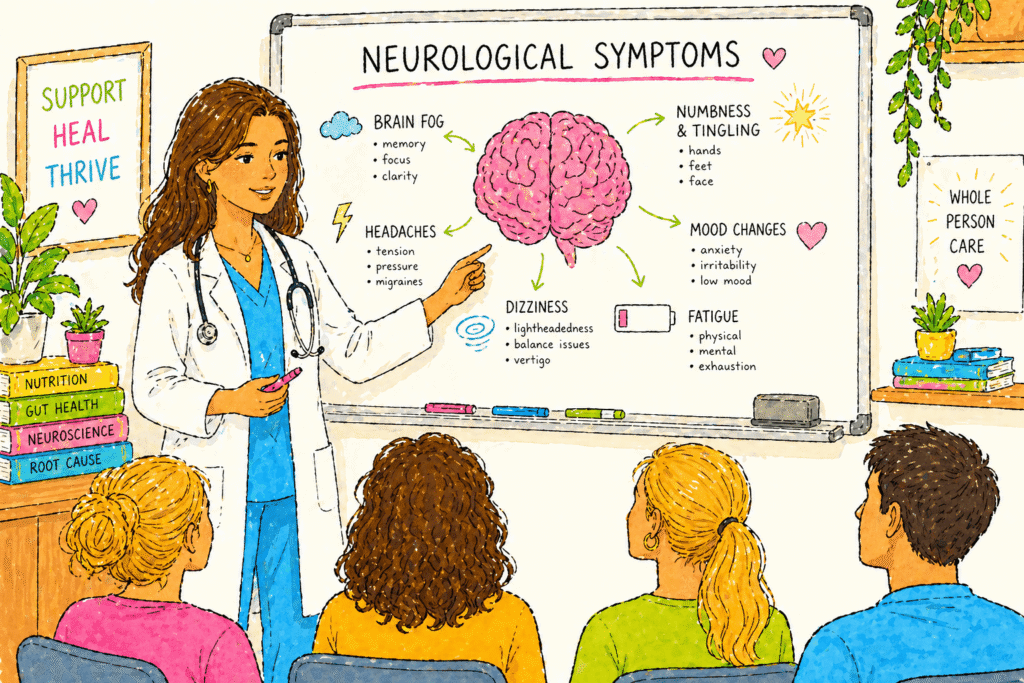
The Full Spectrum of Stage 3 Lyme Disease Neurological Symptoms
Dr. Brian Fallon at Columbia University’s Lyme Disease Research Program has documented an extensive range of neuropsychiatric symptoms associated with Lyme disease through decades of clinical research and objective brain imaging studies.
Stage 3 Lyme disease neurological symptoms include what researchers call Lyme disease brain fog and cognitive impairment, which patients often describe as thinking through cotton wool.
Memory problems are common, including short-term memory loss, difficulty with word retrieval, getting lost in familiar places, and trouble processing information at normal speed.
Mood disturbances including depression, anxiety, emotional instability, and irritability are frequently reported and frequently misattributed to primary psychiatric conditions.
Sleep disturbances, including both insomnia and hypersomnia, can occur alongside night terrors and vivid nightmares.
Neurological symptoms include sensitivity to light and sound, numbness and tingling in the extremities, facial palsy, and in more severe presentations, disorientation and confusion.
A study of 252 Lyme disease patients found that 68 percent showed clinically relevant depressive symptoms on standardized assessment.
Dr. Fallon’s imaging research used objective neurological imaging to demonstrate that these cognitive and mood symptoms have a measurable biological basis, not a psychological one.
They improve when the underlying infection is properly addressed.
This is one of the most important points in this entire article: these are not imaginary symptoms, they are not anxiety, and they are not depression in the conventional sense.
They are the brain’s response to a biological insult that has not been identified or treated.
Co-infections: What Borrelia Brings With It
Borrelia does not typically travel alone.
The same ticks that carry Borrelia frequently carry other pathogens simultaneously, and when multiple infections are present the clinical picture becomes significantly more complex.
In the integrative clinical world, Borrelia is understood as the primary infection that creates the biological terrain in which co-infections can take hold and compound.
Bartonella
Bartonella is one of the most clinically significant co-infections associated with tick-borne illness.
It is endotheliotropic, meaning it has a particular affinity for the endothelial cells that line the blood vessels, including those of the brain.
This vascular colonization can disrupt cerebral blood flow and create neurological symptoms that compound the effects of Borrelia.
A 2024 study conducted by researchers at NC State University and Columbia University Irving Medical Center found that Bartonella DNA was present in the blood of 43 percent of patients with psychosis compared to 14 percent of the control population.
The researchers described this as a potential link warranting further investigation, and called for larger studies to determine whether Bartonella-targeted treatment could improve psychiatric outcomes.
This is emerging research and not yet established as causal.
But it is significant and it points toward questions the conventional psychiatric system has not yet begun to ask.
Babesia
Babesia is a protozoan co-infection that behaves more like malaria than a bacterial infection.
It infects red blood cells and creates a pattern of cyclic symptoms including fever, chills, drenching night sweats, and a distinctive sense of air hunger that many patients describe as one of their most distressing symptoms.
Babesia compounds neurological symptoms by reducing oxygen delivery to the brain through its effects on red blood cells.
It requires a completely different treatment approach than Borrelia and is frequently missed entirely.
Other Factors That Compound the Picture
Beyond tick-borne co-infections, several other conditions frequently occur alongside chronic Lyme disease and worsen the neurological picture.
Thyroid dysfunction, particularly hypothyroidism, is common in people with chronic Lyme disease and contributes independently to the experience of brain fog, depression, cognitive slowing, and fatigue.
Autoimmune processes triggered by chronic infection can create additional neurological inflammation.
Mold toxicity and heavy metal accumulation are frequently found in the chronic Lyme patient population and add to the overall toxic burden the brain is carrying.
This is due to the weakening of the system from the master orchestrator behind it all, Borrelia.
Addressing these additional factors alongside the primary infection is a central principle of integrative Lyme disease treatment.
The Diagnostic Crisis: Why Stage 3 Lyme Disease Neurological Symptoms Are Missed
Given everything we have covered, the diagnostic crisis around stage 3 Lyme disease neurological symptoms begins to make sense.
A patient presents to their doctor with what researchers call Lyme disease brain fog, depression, memory problems, and anxiety.
Standard Lyme testing comes back negative because the biofilm has suppressed the antibody response.
The neurological symptoms are attributed to a primary psychiatric condition.
Psychiatric medication is prescribed.
The medication does not help because it is addressing the wrong problem.
The patient is told the symptoms are psychological.
And the Borrelia in the brain tissue continues its quiet progression, untreated and unacknowledged.
This pattern repeats itself in practitioners’ offices every single day.
Not because the doctors are incompetent.
Because the standard diagnostic tools were not designed to catch what Borrelia, in its late disseminated stage, actually looks like.

What Comprehensive Testing Looks Like
If you suspect stage 3 Lyme disease neurological symptoms may be contributing to a clinical picture that has not responded to conventional treatment, here is what a more thorough evaluation might include.
Standard two-tier testing using ELISA and Western Blot detects antibodies produced by the immune system.
This approach has documented limitations, particularly in late stage disease where Borrelia’s biofilm mechanisms can suppress the antibody response below detectable levels.
TickPlex is a specialized ELISA-based test that differs from standard testing in one important way: it includes antigens for Borrelia’s round body or persister forms, the dormant structures that standard testing cannot detect.
Published research cited in Frontiers in Medicine describes TickPlex as useful across different stages of Lyme disease.
It has been validated using 432 characterized tick-borne disease specimens and is CE and IVD marked for professional laboratory use.
The ELISPOT-LTT, or Lymphocyte Transformation Test, takes a different approach entirely.
Rather than looking for antibodies, it exposes a patient’s lymphocytes to Borrelia antigens and measures whether the immune system’s T-cells react.
A reaction suggests the immune system has encountered Borrelia before.
Some Lyme-literate practitioners use this alongside antibody testing to get a more complete picture of immune activity.
The research on this test is still evolving and results should always be interpreted alongside clinical findings by an experienced practitioner.
Co-infection testing including panels for Bartonella, Babesia, Ehrlichia, and Anaplasma is recommended alongside any Lyme testing.
A complete thyroid panel, comprehensive metabolic panel, and assessment of heavy metal and mycotoxin burden round out a thorough evaluation for anyone presenting with complex neurological symptoms that have not responded to standard care.
Working with a Lyme-literate integrative practitioner who understands the full picture of tick-borne illness remains essential.
These are specialized tools that require experienced clinical interpretation.
If your neurological or psychiatric symptoms have not responded to conventional treatment, if they wax and wane in cycles, if they appeared following a period of outdoor exposure or an unexplained flu-like illness, Lyme disease and its co-infections deserve serious consideration as a root cause.
FAQ Stage 3 Lyme disease Neurological Symptoms
What are stage 3 Lyme disease neurological symptoms?
Stage 3 Lyme disease, also called late disseminated Lyme disease, refers to infection that has spread to the nervous system and brain.
Stage 3 Lyme disease neurological symptoms include the experience of Lyme disease brain fog, cognitive impairment, short-term memory loss, difficulty with word retrieval, depression, anxiety, mood swings, sleep disturbances, sensitivity to light and sound, numbness and tingling, and in more severe cases, disorientation and neuropsychiatric presentations.
These symptoms can appear months to years after the initial infection and are frequently misdiagnosed as primary psychiatric conditions.
Can Lyme disease cause brain fog?
Yes. The experience of Lyme disease brain fog is one of the most commonly reported stage 3 Lyme disease neurological symptoms.
Patients describe it as thinking through cotton wool, an inability to find words, slow processing speed, and difficulty holding multiple thoughts at once.
Research at Columbia University using objective neurological imaging has demonstrated that what researchers call Lyme disease brain fog has a measurable biological basis and responds when the underlying infection is properly supported.
Why does standard Lyme testing miss so many cases?
Standard Lyme testing detects antibodies produced by the immune system in response to Borrelia infection.
However, Borrelia’s biofilm formation can suppress the immune response and alter antigen expression, resulting in antibody levels below detectable thresholds.
Additionally, Borrelia uses antigenic variation to continuously change its surface proteins, making it harder for the immune system to mount a consistent antibody response.
Research has documented the sensitivity of standard two-tier Lyme testing at between 34 and 70 percent, depending on the stage of disease, meaning a significant number of infected patients receive false negative results.
What is neuroborreliosis?
Neuroborreliosis is the term used to describe Lyme disease that has affected the nervous system.
It is a recognized clinical diagnosis that encompasses the full range of stage 3 Lyme disease neurological symptoms.
Neuroborreliosis can involve both the central nervous system (brain and spinal cord) and the peripheral nervous system (nerves throughout the body).
It has been confirmed in post-mortem brain tissue analysis and in cerebrospinal fluid studies in living patients.
How does Borrelia hide from the immune system?
Borrelia uses several sophisticated immune evasion strategies.
It forms biofilm, a protective polysaccharide matrix that shields it from both immune attack and antibiotic penetration.
It uses antigenic variation to continuously change its surface proteins, staying one step ahead of immune recognition.
It can transform into metabolically inactive round body forms that are resistant to antibiotics.
And it can invade and persist inside human cells including neural cells, where standard immune surveillance has difficulty reaching.
These mechanisms together make Borrelia one of the most challenging bacterial pathogens to detect and eradicate.
What co-infections should be tested for alongside Lyme disease?
The most clinically significant co-infections to test for alongside Lyme disease are Bartonella, Babesia, Ehrlichia, and Anaplasma.
These pathogens are transmitted by the same ticks that carry Borrelia and are frequently present simultaneously.
Each requires a different treatment approach and each can contribute independently to neurological and psychiatric symptoms.
A comprehensive co-infection panel through a specialized laboratory is recommended for anyone with suspected late stage or treatment-resistant Lyme disease.
Related Reading on Dodhisattva
If this article resonated with you, you may also find these posts helpful:
Chronic Lyme Disease Natural Treatment: The Holistic Protocol Most Doctors Have Never Heard Of
Bartonella Symptoms: What This Hidden Co-Infection Is Doing to Your Body
Babesia Symptoms: The Malaria-Like Co-Infection Most Doctors Miss
The Neck as Your Body’s Hidden Highway: Cervical Lymphatic Drainage and Lyme Recovery
Research and Sources
Golovchenko M, et al. Concurrent Infection of the Human Brain with Multiple Borrelia Species. Int J Mol Sci. 2023 Nov 29;24(23):16906. https://www.mdpi.com/1422-0067/24/23/16906
Gadila et al. Detecting Borrelia Spirochetes: A Case Study With Validation Among Autopsy Specimens. Frontiers in Neurology. 2021. https://www.frontiersin.org/journals/neurology/articles/10.3389/fneur.2021.628045/full
Delaney S, et al. Bartonella species bacteremia in association with adult psychosis. Front Psychiatry. 2024. https://pmc.ncbi.nlm.nih.gov/articles/PMC11190357/
Bransfield RC. Neuropsychiatric Lyme Borreliosis: An Overview with a Focus on a Specialty Psychiatrist’s Clinical Practice. Healthcare. 2018. https://pmc.ncbi.nlm.nih.gov/articles/PMC6165408/
Buhner SH. Healing Lyme: Natural Healing of Lyme Borreliosis and the Coinfections Chlamydia and Spotted Fever Rickettsioses. Raven Press. 2015.
Lacout A, et al. Biofilms busters to improve the detection of Borrelia using PCR. Med Hypotheses. 2018. https://www.sciencedirect.com/science/article/abs/pii/S030698771731037X
Cook MJ, Puri BK. Commercial test kits for detection of Lyme borreliosis: a meta-analysis of test accuracy. Int J Gen Med. 2016.
Neuropsychiatric and Psychological Symptoms in Patients with Lyme Disease: A Study of 252 Patients. PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC8232147/
About Author
If something here resonated with you, I invite you to learn more about the philosophy and clinical training behind this work. Visit the About page to understand where this knowledge comes from and why it is different from anything else you will find online.POPULAR POSTS