ENTER THE SACRED BACKYARD
SACRED SOUL FAMILY

Dodee is a Certified Holistic Health Practitioner, Autonomic Response Testing Practitioner, and Biofield Science Educator with nearly two decades of experience in chronic illness recovery and integrative wellness. Dodhisattva.com, est. 2009
Tick bite symptoms are easy to miss, and that is exactly what makes them so consequential.
Most people who are eventually diagnosed with Lyme disease or a tick-borne co-infection did not recognize what was happening in the days and weeks after a bite.
Some never found the tick at all.
Others noticed a small redness that faded and assumed everything was fine.
Understanding what tick bite symptoms actually look like, including the presentations that do not match the classic picture, is one of the most important things anyone who spends time outdoors can know.
Ticks do not simply bite and leave.
They are designed to feed undetected for extended periods, sometimes days, which is why their bites are often painless and go unnoticed.
When a tick attaches to the skin it uses its hypostome, a barbed feeding tube, to anchor itself and begin drawing blood.
As it feeds it secretes saliva containing compounds that suppress the local immune response, numb the bite site, and in infected ticks, deliver the pathogens that cause tick-borne illness.
Borrelia burgdorferi, the spirochete bacteria behind Lyme disease, uses the immunomodulatory properties of tick saliva to increase its ability to establish infection and evade the initial immune response.
This is part of why early tick bite symptoms can be so subtle and why recognizing them quickly matters.
The longer a tick remains attached the greater the opportunity for pathogen transmission.
Literature often notes that the risk of transmission is frequently observed to increase after extended attachment periods, though this window varies depending on the pathogen and the tick species involved.

Not every tick bite produces symptoms.
A bite from an uninfected tick may cause nothing more than a small red mark that resolves within a day or two.
The presence of symptoms signals that something more is happening and deserves attention.
A small bump or redness at the site of a tick bite is common and normal immediately after removal.
This is an inflammatory reaction to the mechanical bite itself and typically resolves within one to two days.
This early reaction is not a sign of Lyme disease on its own.
An allergic reaction to tick saliva can also occur at the bite site.
This typically appears within 72 hours, remains smaller than two inches in diameter, and fades within a few days.
It is distinguishable from the Lyme rash by its limited size and short duration.
The erythema migrans rash is the most recognized early of the tick bite symptoms and appears in approximately 70 to 80 percent of people infected with Lyme disease.
It typically develops between three and thirty days after the bite, with most cases appearing within three to ten days.
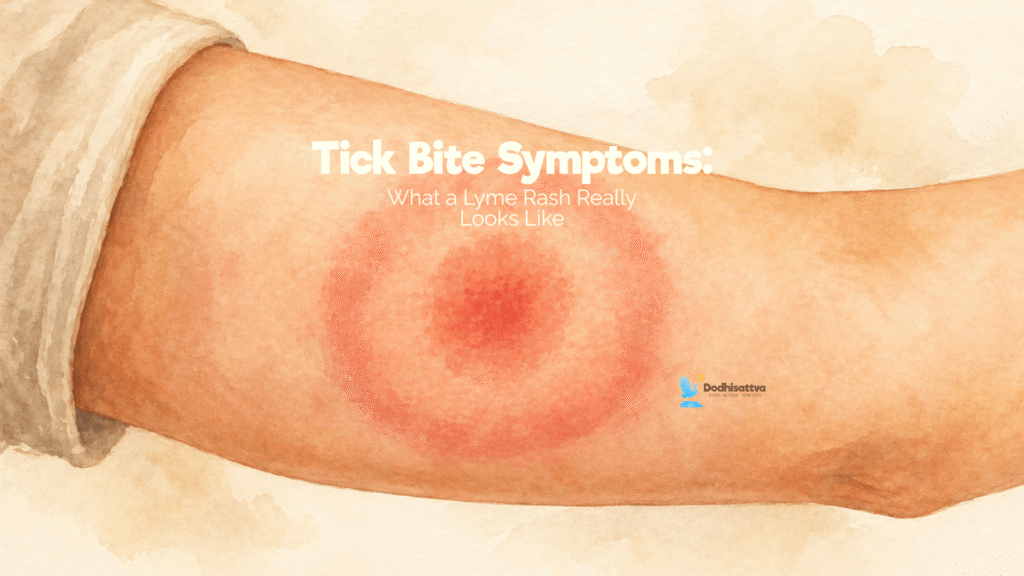
One of the most important things to understand about the Lyme disease rash is that the classic bull’s eye pattern, a red ring surrounding a clear area with a red center, is actually present in only a minority of cases.
Research from Johns Hopkins Lyme Disease Research Center clarifies that the most common tick bite symptoms present as a uniformly red, round or oval rash that expands over days to a diameter greater than two inches.
It is often six to eight inches at its widest.
The rash is typically minimally tender and minimally itchy, much less itchy than poison ivy, and sometimes warm to the touch.
It expands progressively rather than staying the same size.
A rash that stays small and fades within a few days is more likely an allergic reaction than erythema migrans.
Sometimes blisters develop in the center of the rash.
In some cases the bacteria spread through the bloodstream and create additional erythema migrans lesions at sites distant from the original bite.
Individuals often report that early patterns associated with tick bite symptoms & exposure can extend beyond the skin.
According to NIH StatPearls, early localized Lyme disease commonly produces flu-like symptoms alongside or without the rash, including fatigue, malaise, headache, fever, chills, muscle aches, joint pain, and swollen lymph nodes.
These symptoms can appear even in the absence of a visible rash.
Research published in NCBI Bookshelf notes that flu-like symptoms including fever, headache, drowsiness, and aching muscles appearing within six weeks of a tick bite should prompt medical attention even without a skin rash.
The difficulty is that these symptoms overlap significantly with common viral illnesses, which is one of the primary reasons Lyme disease is frequently missed or delayed in diagnosis.
What distinguishes them in context is the recent history of a tick bite or time spent in tick habitat.
When tick-borne infection is not addressed in the early stage the bacteria can disseminate through the bloodstream to joints, the heart, the nervous system, and other organs.
The CDC describes this progression through three stages: early localized, early disseminated, and late disease.
According to the CDC, the erythema migrans rash appears in the majority of Lyme disease cases and is the most recognized early sign of infection.
Early disseminated tick bite symptoms, developing weeks to months after the initial bite, can include multiple erythema migrans lesions appearing at sites away from the original bite, facial palsy or Bell’s palsy affecting one or both sides of the face, heart palpitations or irregular heartbeat known as Lyme carditis, nerve pain, numbness or weakness in the arms or legs, and severe headache with stiff neck.
Later stage symptoms can include severe joint pain and swelling particularly affecting the knees and other large joints, neurological symptoms including cognitive impairment and memory difficulties, extreme fatigue, and central nervous system dysfunction.
Johns Hopkins Lyme Disease Research Center notes that late disseminated Lyme disease has a wide range of presentations and that the bacteria can travel through the bloodstream to joints, the heart, the brain, muscles, and the nervous system when early infection goes unaddressed.
One of the most underappreciated aspects of tick bite symptoms is that a single tick bite can transmit more than one pathogen simultaneously.
Co-infections with organisms like Bartonella and Babesia are well documented and significantly complicate the clinical picture.
Bartonella, sometimes called cat scratch disease in its more common form, is a bacterial co-infection that has been found in ticks alongside Borrelia.
Research has documented Bartonella in the endothelial cells lining blood vessels throughout the body.
Symptoms that may be associated with Bartonella co-infection include a distinctive linear rash sometimes described as stretch mark-like striations, neurological symptoms, fatigue, and lymph node involvement.
Babesia is a parasitic co-infection that lives inside red blood cells and operates similarly to malaria.
The signature symptom pattern of Babesia includes air hunger, a sensation of being unable to take in enough breath, drenching night sweats that cycle with fever and chills, and deep fatigue.
A 2015 report noted that up to 40 percent of Lyme disease patients may also have Babesia co-infection.
When co-infections are present tick bite symptoms become more varied, more persistent, and more difficult to attribute to a single cause.
This is one of the reasons that integrative practitioners working with tick-borne illness look at the full picture of symptoms rather than testing for a single organism.

Finding an attached tick warrants prompt and careful removal.
The recommended approach is to use fine-tipped tweezers, grasp the tick as close to the skin surface as possible, and pull upward with steady even pressure without twisting or jerking.
Avoid crushing the tick’s body.
After removal, clean the bite area with rubbing alcohol or soap and water.
Note the date of the bite and monitor the site for the development of a rash over the following two to four weeks.
Photograph any rash that appears to document its size and progression.
Seek prompt medical attention if a rash develops, if flu-like symptoms appear within six weeks of the bite, or if there is any concern about the duration of attachment or the type of tick involved.
From an integrative perspective, the period immediately following a tick bite is viewed as a window of opportunity to support the body’s immune response before any infection has the chance to establish itself.
Andrographis paniculata is one of the herbs most commonly discussed in integrative tick-borne illness protocols.
It has documented anti-inflammatory and immune supporting properties and is sometimes described as the first herb practitioners reach for in the context of tick exposure.
It has been studied for its role in supporting the body’s natural response to bacterial and inflammatory markers.
Supporting drainage pathways through the lymphatic system is considered foundational in integrative approaches to tick-borne illness.
The lymphatic system is responsible for clearing pathogens and inflammatory debris from tissues throughout the body.
Practices that support lymphatic flow include movement, hydration, and specific botanical support.
These are not treatments for tick-borne disease.
They are approaches that integrative practitioners observe as supportive of immune function and overall terrain during a period of potential exposure.
Anyone who suspects tick-borne infection should work with a qualified health practitioner for appropriate evaluation and guidance.
You can read more in our article: Is there a Natural Remedy for Lyme Disease?
The challenge with tick-borne illness is that its early presentation is easy to dismiss.
A rash that fades, a week of feeling run down, joint aches that seem like they might be from something else.
By the time more serious symptoms develop the window for straightforward early support has often passed.
Understanding tick bite symptoms and taking them seriously in the acute phase is one of the most meaningful things a person can do for their long-term health after a tick exposure.
If you recognize yourself in the symptom picture described in this article, whether from a recent bite or a history of unexplained illness following tick exposure, the most important step is working with a practitioner experienced in tick-borne illness who can help you get appropriate evaluation and build a protocol tailored to your specific picture.
Tick bite symptoms are real, they are varied, and they deserve to be taken seriously from the very first sign.
Chronic Lyme Disease Natural Treatment: The Holistic Protocol Most Doctors Have Never Heard Of
Bartonella Symptoms: What This Hidden Co-Infection Is Doing to Your Body
Babesia Symptoms: The Malaria-Like Co-Infection Most Doctors Miss
The Neck as Your Body’s Hidden Highway: Cervical Lymphatic Drainage and Lyme Recovery
Sources
1. Bratton RL et al. Tick-Borne Disease. StatPearls. NIH NCBI. https://www.ncbi.nlm.nih.gov/books/NBK431066/
2. Centers for Disease Control and Prevention. Signs and Symptoms of Untreated Lyme Disease. https://www.cdc.gov/lyme/signs-symptoms/index.html
3. Johns Hopkins Lyme Disease Research Center. Lyme Disease Symptoms. https://www.hopkinslyme.org/lyme-disease/lyme-disease-signs-symptoms/
4. NCBI Bookshelf. Tick Bites: Lyme Disease. InformedHealth.org. https://www.ncbi.nlm.nih.gov/books/NBK279242/
5. PMC. Cutaneous Manifestations of Lyme Borreliosis in Children. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9864164/
6. PMC. Erythema nodosum as first clinical sign of acute Borrelia burgdorferi infection. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC11693426/
7. MedlinePlus. Lyme Disease. National Library of Medicine. https://medlineplus.gov/lymedisease.html
Disclaimer: This article is for educational and informational purposes only. It is not intended to diagnose, treat, cure, or prevent any disease. Always work with a qualified healthcare practitioner for any health concerns.

POPULAR POSTS
MEDITATIONS
It’s FREE! And I know you’re going to love it.